Surgery
Cataracts
Cataracts are characterized by the opacification of the crystalline lens, the natural, transparent lens of the eye that enables us to see. When the crystalline lens becomes opaque, vision becomes blurred. This phenomenon, known as cataract, generally begins around the age of 65. However, it can also develop at a younger age as a result of metabolic diseases such as diabetes.
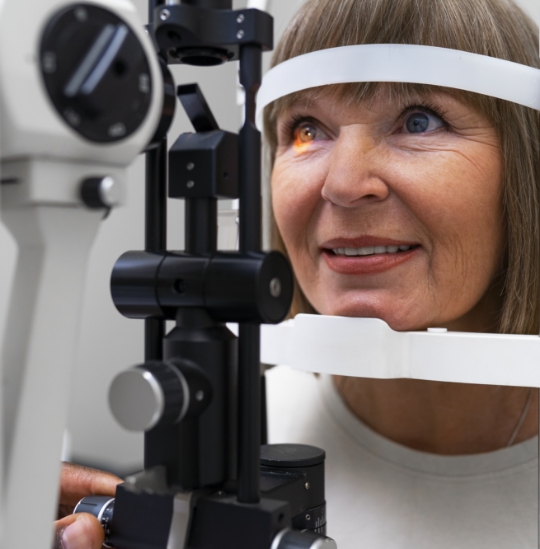
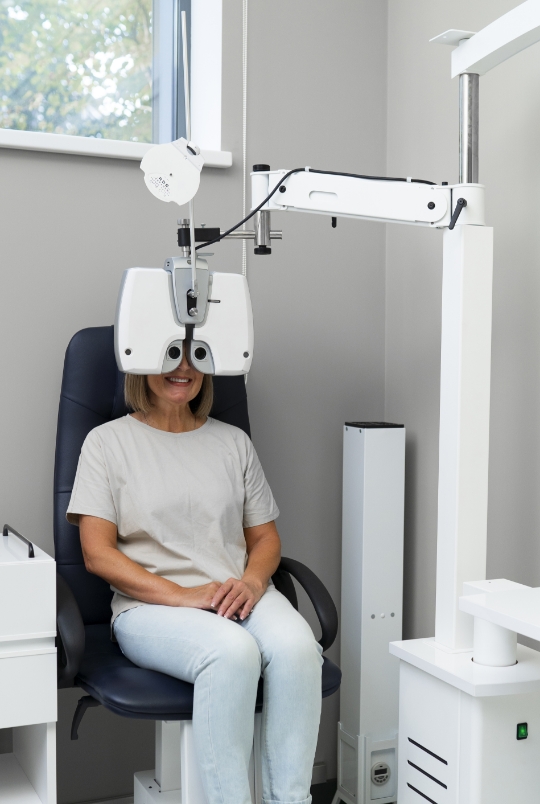
Treatment
Purpose of the operation
cataract
Cataract surgery at Vision Future Switzerland is subject to constant technological innovation. Its main aim is to replace the opacified crystalline lens with an artificial lens, known as an intraocular implant.
Three key points demonstrate the importance of this procedure:
- Improves vision by restoring lens transparency
- Artificial lens selection to correct pre-existing vision anomalies
- Choice of premium, fully customized implants to correct refractive anomalies

Treatments
Intraocular implants
Multifocal implants
These implants correct both distance and near vision (presbyopia), and are indicated for patients without astigmatism.
Operation sequence
Surgery
cataract
Preoperative examination :
Lens removal :
Implant insertion :
An implant will be inserted to replace the opaque lens responsible for the cataract.
Post-operative follow-up :
You'll need to rest and follow the instructions of the Vision Future teams.
Our specialists
Our team of experts in FMH Ophthalmology
and Ophthalmic Surgery FMH
Find out more about our experienced ophthalmologists.

Doctor
Marouen Berguiga
Specialist FMH
in Ophthalmology
and Ophthalmic Surgery
Eye diseases
- Treatment of visual disorders in children and adults
Anterior segment surgery
- Cataract surgery
- Glaucoma surgery
- Refractive surgery
- Corneal transplant
- Oculoplastic surgery
- Management of keratoconus
- Intravitreal injections
Medical retinal treatment
Languages spoken :
French, English, Italian, Arabic

Doctor
Khaled Romdhane
Specialist FMH
in Ophthalmology
and Ophthalmic Surgery
Eye diseases
- Treatment of visual disorders in children and adults
- Management of retinal diseases
- Management of glaucoma diseases
Anterior segment surgery
- Cataract surgery
- Refractive surgery
- Intravitreal injections
- Angiography
Medical retinal treatment
Languages spoken :
French, English, Arabic

Doctor
Horace Massa
Specialist FMH
in Ophthalmology
and Ophthalmic Surgery
Eye diseases
- Treatment of visual disorders in children and adults
Anterior segment surgery
- Cataract surgery
- Glaucoma surgery
- Refractive surgery
- Corneal transplant
- Oculoplastic surgery
- Management of keratoconus
- Intravitreal injections
Medical retinal treatment
Languages spoken :
French, English, German, Italian

Docteur
Augustina Grigaite
Specialist FMH
in Ophthalmology
and Ophthalmic Surgery
Eye diseases
- Treatment of visual disorders in adults
Anterior segment surgery
- Cataract surgery
- Refractive surgery
Languages spoken :
French, English, German, Italian, Russian, Lithuanian
Make an appointment at the clinic
Appointments can be booked directly on our website or via the OneDoc app.
Appointments for laser surgery can only be made via our WhatsApp line.
In case of emergency, please contact us directly on 022 365 18 80
FAQ
Some quick answers to your questions
What are the most common symptoms?
How is cataract treated?
The treatment for cataracts is surgery. The decision to undergo cataract surgery is usually based on the patient's functional visual impairment.
When does a cataract occur?
Cataracts generally begin at the age of 65, but can also occur at a younger age as a result of metabolic diseases such as diabetes, prolonged use of corticosteroids or eye trauma.